Far Infrared Thermal Therapy,
Hippocrates Health Institute, Florida.
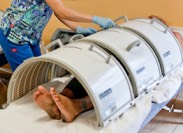
Pure
far infrared is a 'dry' heat used in close
proximity to the body for optimal penetration, as
can be seen in the large thermal therapy
'incubation' units used in European health
clinics. Clothing does not have to be removed.
Anyone who has received thermal
therapy in Europe will attest it is not
inexpensive - clinic fees, hotel cost, travel
expenses etc - but results are often worthwhile.
However, for those wishing to use
thermal therapy units in their home, it must be
advised that ...
a) Research must be done to
find a unit that will provide optimal benefits.
b) Thermal therapy is an intergrative
modality that may safely be used alongside
conventional protocols if so desired.
c) Emotions and diet MUST be
addressed
d) Suitable health care practitioners
(those educated in far infrared therapy) should
be consulted on the healing journey to recovery
for guidance if needed.
Important Note:
American Far Infrared
units.
When reading the American NCI document below,
please keep in mind that these American methods are really
crude, and even involve probes which can
burn the body. Side effects using American methods
discussed below, are quite frankly completely
undesirable and frightening.
Asian and European Far
Infrared units
(not traditional saunas which generate wet heat
with ineffective far infrared), are far more
advanced and do not use probes,
therefore there is no damage to the body of any
kind, just pure Far Infrared dry heat which does NOT
burn or harm the body, but heal and strengthen it!
NCI Fact Sheet:
Experimental
applications and results using hyperthermia.
What is hyperthermia?
"Hyperthermia
(also called thermal therapy or thermotherapy) is
a type of cancer therapy in which body tissue is
exposed to high temperatures (up to 113°F).
Research has shown that high temperatures can
damage and kill cancer cells, usually with minimal
injury to normal tissues
(1)
By killing cancer cells and damaging proteins and
structures within cells
(2), hyperthermia may shrink tumors.
Hyperthermia is under study in clinical trials
(research studies with people) and is not widely
available (in the U.S.).
How is
hyperthermia used to treat cancer?
Hyperthermia is almost always used with other
forms of cancer therapy, such as radiation therapy
and chemotherapy (1, 3). Hyperthermia may make
some cancer cells more sensitive to radiation or
harm other cancer cells that radiation cannot
damage.
When
hyperthermia and radiation therapy are combined,
they are often given within an hour of each other.
Hyperthermia can also enhance the effects of
certain anticancer drugs.
Numerous
clinical trials have studied hyperthermia in
combination with radiation therapy and/or
chemotherapy.
These studies have focused on the
treatment of many types of cancer, including
sarcoma, melanoma, and cancers of the head and
neck, brain, lung, esophagus, breast, bladder,
rectum, liver, appendix, cervix, and peritoneal
lining (mesothelioma) (1, 3-7).
Many of these studies, but not all,
have shown a significant reduction in tumor size
when hyperthermia is combined with other
treatments (1, 3, 6, 7).
However, not all of these studies have
shown increased survival in patients receiving
the combined treatments (3, 5, 7).
What are the
different methods of hyperthermia?
Several methods of hyperthermia are currently
under study, including local, regional, and
whole-body hyperthermia (1, 3-9).
In local hyperthermia, heat is applied to a small
area, such as a tumor, using various techniques
that deliver energy to heat the tumor. Different
types of energy may be used to apply heat,
including microwave, radio frequency, and
ultrasound. Depending on the tumor location, there
are several approaches to local hyperthermia:
External
approaches are used to treat tumors that are in or
just below the skin.
External
applicators are positioned around or near the
appropriate region, and energy is focused on the
tumor to raise its temperature.
Intraluminal
or endocavitary methods may be used to treat
tumors within or near body cavities, such as the
esophagus or rectum. Probes are placed inside the
cavity and inserted into the tumor to deliver
energy and heat the area directly.
Interstitial
techniques are used to treat tumors deep within
the body, such as brain tumors. This technique
allows the tumor to be heated to higher
temperatures than external techniques.
Under
anesthesia, probes or needles are inserted into
the tumor. Imaging techniques, such as ultrasound,
may be used to make sure the probe is properly
positioned within the tumor. The heat source is
then inserted into the probe.
Radio
frequency ablation (RFA) is a type of interstitial
hyperthermia that uses radio waves to heat and
kill cancer cells.
In
regional hyperthermia, various approaches may be
used to heat large areas of tissue, such as a body
cavity, organ, or limb. Deep tissue approaches may
be used to treat cancers within the body, such as
cervical or bladder cancer.
External
applicators are positioned around the body cavity
or organ to be treated, and microwave or radio
frequency energy is focused on the area to raise
its temperature.
Regional perfusion techniques can be used to focus
on cancers in the arms and legs, such as melanoma,
or cancer in some organs, such as the liver or
lung. In this procedure, some of the patient’s
blood is removed, heated, and then pumped
(perfused) back into the limb or organ. Anticancer
drugs are commonly given during this time.
Continuous
hyperthermic peritoneal perfusion (CHPP) is a
technique used to treat cancers within the
peritoneal cavity (the space within the abdomen
that contains the intestines, stomach, and liver),
including primary peritoneal mesothelioma and
stomach cancer.
During
surgery, heated anticancer drugs flow from a
warming device through the peritoneal cavity. The
peritoneal cavity temperature reaches 106-108°F.
Whole-body hyperthermia is used to treat
metastatic cancer that has spread throughout the
body. This can be accomplished by several
techniques that raise the body temperature to
107-108°F, including the use of thermal chambers
(similar to large incubators) or hot water
blankets.
The
effectiveness of hyperthermia treatment is related
to the temperature achieved during the treatment,
as well as the length of treatment and cell and
tissue characteristics (1, 2).
To
ensure that the desired temperature is reached,
but not exceeded, the temperature of the tumor and
surrounding tissue is monitored throughout
hyperthermia treatment (3, 5, 7).
Using
local anesthesia, the doctor inserts small needles
or tubes with tiny thermometers into the treatment
area to monitor the temperature. Imaging
techniques, such as CT (computed tomography), may
be used to make sure the probes are properly
positioned (5).
Does hyperthermia
have any complications or side effects?
Most normal tissues are not damaged
during hyperthermia if the temperature remains
under 111°F. However, due to regional differences
in tissue characteristics, higher temperatures may
occur in various spots.
This
can result in burns, blisters, discomfort, or pain
(1, 5, 7). Perfusion techniques can cause tissue
swelling, blood clots, bleeding, and other damage
to the normal tissues in the perfused area;
however, most of these side effects are temporary.
Whole-body
hyperthermia can cause more serious side effects,
including cardiac and vascular disorders, but
these effects are uncommon (1, 3, 7). Diarrhea,
nausea, and vomiting are commonly observed after
whole-body hyperthermia (7).
What does
the future hold for hyperthermia?
A number of challenges must be
overcome before hyperthermia can be considered a
standard therapy for cancer (1, 3, 6, 7). Many
clinical trials are being conducted to evaluate
the effectiveness of hyperthermia.
Some
trials continue to research hyperthermia in
combination with other therapies for addressing
different cancers. Other studies focus on improving
hyperthermia techniques.



